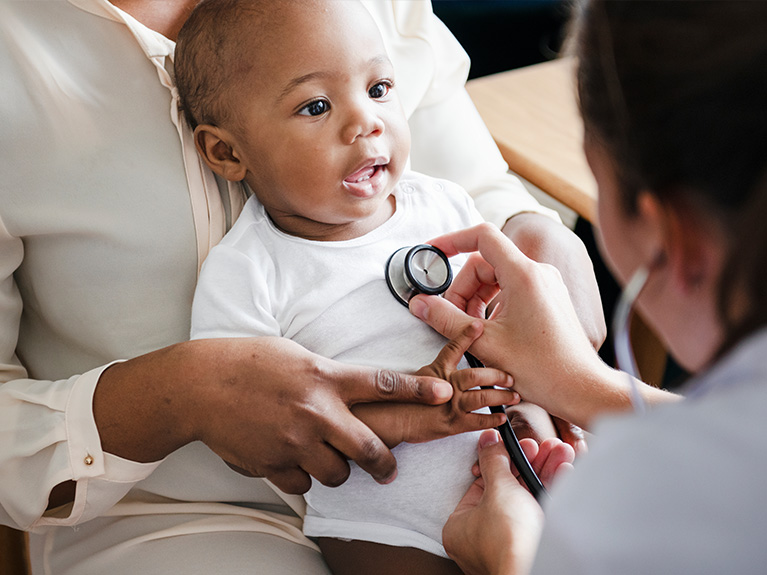
 C-TAC hosted a mixer on July 25 highlighting the need to include the pediatric voice in serious illness care. The discussion focused on pivotal policy and program solutions to enhance care for children grappling with serious illnesses and their families.
C-TAC hosted a mixer on July 25 highlighting the need to include the pediatric voice in serious illness care. The discussion focused on pivotal policy and program solutions to enhance care for children grappling with serious illnesses and their families.
Leaders Address the Pediatric Gap
Bill Novelli, C-TAC co-founder and co-board chair, kicked off the event noting,
“The job of the Coalition is to serve as a voice and a catalyst for the growing movement in advanced illness care. As this movement continues to gain momentum, C-TAC recognizes the need to encompass pediatrics within its broader scope.”
Betsy Hawley, executive director of the Pediatric Palliative Care Coalition, led the discussion, highlighting significant policy advancements in pediatric care but noted much more needs to be done.
Dr. Dominic Moore, a C-TAC board member and Division Chief for Pediatric Palliative Care at the University of Utah School of Medicine, is dedicated to bridging this gap.
He emphasized that, “C-TAC’s goal is only complete when it serves the interests of children and adults. Pediatric care is often left behind in national discussions, and it is inspiring to see C-TAC work to keep our focus on all groups in need of excellent care.”
Kristen James, CEO of the Greater Illinois Pediatric Palliative Care Coalition (PPCC), shared encouraging developments from Illinois, where recent bills mandated home-based pediatric benefits for Medicaid recipients and required similar provisions from private insurers. However, these successes mark just the initial steps, necessitating continued efforts for effective implementation. The PPCC is actively seeking national collaboration to further impact pediatric care.
Capital Caring Kids executive director Allison Kuchar, discussed establishing direct connections with state Medicaid medical directors. These connections have enabled their organization to navigate complex pediatric cases and secure essential care, particularly given the diverse Medicaid coverage landscape.
Dr. Kenneth Pituch, clinical professor emeritus at University of Michigan Health, C.S. Mott Children’s Hospital, highlighted the success of the Michigan Concurrent Hospice and Curative Care for Children policy, which broadened access to concurrent care. This policy’s interpretation of what qualifies as a life limiting diagnosis has enabled many patients to receive the concurrent care they need without pushback from Medicaid. Dr. Pituch also outlined the expansion of a chronic complex care program piloted at the University of Michigan Children’s Hospital, aiming to provide reimbursement for pediatric patients’ complex care.
The Critical Role of Pediatric Caregivers
Caregiving.com head of community partnerships, Shaina Purser, highlighted the indispensable role of caregivers in policy discussions. She further emphasized that caregivers, especially family members, contribute valuable continuous patient data, making their involvement vital. Additionally, she addressed the need to include respite care for caregivers in those policy discussions.
In response to the concerns raised about the role of and support for caregivers, Tracy Leonard-Warner, executive director of Ryan House, which provides pediatric palliative care and pediatric respite care for families, shared Arizona’s plans to extend the paid caregiver program to address the need to support and recognize the critical role of caregivers in pediatric care.
National Collaborative Efforts
The National Coalition for Hospice and Palliative Care (NCHPC) project director, Devon Dabbs, shared updates from the NCHPC Pediatric Palliative Care Task Force. The task force brings together diverse leaders and parents in the serious illness pediatric space to craft solutions at the national level.
Kristen James highlighted the diversity in hospice providers across the nation, emphasizing the need for adaptable programming. To this point, Torrie Fields, a C-TAC strategic advisor, stressed that the real exercise is getting down some consensus standards on what the minimum set of requirements about the services delivered are. Accomplishing this would enable pediatric benefits to be implemented at a national level and move toward more permanent policies rather than state waivers.
Alex Kuznetsov, senior manager of disabilities and special health care needs at the American Academy of Pediatrics(AAP), detailed efforts to establish pediatric palliative care policies at the national and state levels, ensuring pediatric care issues receive due attention.
And Laura Bryant-Earner, service director at Healwell, described how her organization is leading efforts to incorporate massage therapy into patient care and support for caregivers.
C-TAC is the voice of the patient and family impacted by serious illness. To learn more about how you can become a member of C-TAC, contact Luke Scuitto, Partnership Director at LScuitto@thectac.org or Sandra Arias, Partnership Associate at SArias@thectac.org



